REGULATION OF MINERAL METABOLISM:
PTH and 1, 25-dihydroxyvitamin D
are the primary hormones regulating bone and mineral metabolism. Physiological
role of calcitonin has not yet been established. PTHrP is the principal
mediator of humoral hypercalcemia of malignancy.
PARATHYROID HORMONE
PTH (chromosome 11) is synthesized
and secreted by parathyroid glands located posterior to thyroid gland. The glands
consist of chief and oxyphil cells; the chief cells synthesize, store, and
secrete PTH. It is cleared by liver and kidney. PTH acts directly on bone and
kidney, and indirectly on intestine to regulate concentration of calcium and
phosphate in plasma.
PTH is synthesized as pre-pro-PTH
of 115 amino acids. These pre and pro segments are cleaved during their
transport to GA where intact 84 amino acid PTH is formed. It is then stored,
secreted or degraded intracellularly. PTH acts on the receptor and produce
biological response like calcemic, phosphaturic and other response in kidney
and bone. Oxidation of methionine residue at position 8 or 18 results in loss
of biological activity. The middle portion of the molecule is quite immunogenic
because of its hydrophobicity and species specificity. Further cleavage at
C-terminal inactivates the hormone.
Free calcium in extracellular fluid
is the main regulator of PTH synthesis, secretion and metabolism. Parathyroid
gland responds to decrease in free calcium concentration within seconds. Calcium
interacts with plasma membrane G protein coupled receptor in parathyroid cells;
this leads to release of free calcium from intracellular stores and opening of
membrane bound calcium channels. Hypercalcemia inhibits PTH synthesis and
secretion and increases PTH metabolism whereas hypocalcemia has opposite
effect.
1, 25-dihydroxyvitamin-D, phosphate
and magnesium also influences the synthesis and secretion of PTH. Vitamin D
interacts with vitamin D receptors in the parathyroid glands to chronically suppress
PTH synthesis by suppressing PTH gene transcription and therefore secretion.
Hyperphosphatemia and hypophosphatemia increase and decrease PTH synthesis and
secretion respectively. Chronic severe hypomagnesemia such as in occurring in
alcoholism has been associated with impaired PTH secretion, whereas acute
hypomagnesemia may stimulate secretion. Hypermagnesemia suppress PTH secretion
via the calcium sensing receptor in parathyroid gland.
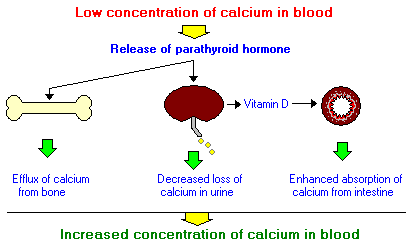
PTH influences both calcium and
phosphate homeostasis directly through its actions on both bone and kidney and
indirectly on the intestine through 1, 25(OH)2D. PTH acts on its
receptor and activates adenylyl cyclase producing cAMP, activation of kinase,
phosphorylation of proteins, increased entry of calcium and releases intracellular
calcium, stimulated phospholipase C activity with generation of DAG and
phosphoinositide activated enzyme and transport systems, and secretion of
lysosomal enzymes.
In the kidneys, PTH (1) induces
25-hydroxyvitamin D-1α-hydroxylase, increasing the production of 1, 25 (HO)2D,
which stimulates intestinal absorption of both calcium and phosphate, (2)
increases calcium reabsorption in the DCT of nephron, (3) decreases
reabsorption of phosphate by PCT, and (4) inhibits Na+-H+
antiporter activity, which favors a mild hyperchloremic metabolic acidosis in
hyperparathyroid states.
The effects of PTH on bone are
chronic exposure to high concentration of PTH leads to increased bone
resorption. It acts by altering the activity and number of osteoblasts and
osetoclasts. Bone resorption a prompt effect, is important for maintenance of
calcium homeostasis, whereas delayed effect are important for extreme systemic
needs and skeletal homeostasis.
Thus all these conditions lead to
increase in free and total calcium in serum but decreased phosphate. In urine
inorganic phosphate and cAMP are increased. The increase in serum calcium
reduces PTH secretion through a negative feedback loop, maintaining
homeostasis.
Biologically active intact PTH is
rapidly cleared from plasma (half-life<5 minutes) by metabolism to
C-terminal fragments by liver and kidneys and cleared of intact PTH by kidneys.
But rate of degradation of PTH decreases when calcium concentrations are low
and increases when calcium is high.



No comments:
Post a Comment